Categories
Select a new category
Traits of Kids Diagnosed with ASD after Passing M-CHAT
By Chelsea Toledo, M.A. on September 18, 2018

Background: Diagnosis of ASD requires systematic and structured observation of a child by trained clinicians. While the diagnostic process is comprehensive, the first step is a screening – known as the Modified Checklist for Autism in Toddlers (M-CHAT) – that takes place at children’s regular pediatric appointments when they are 18 months old.
What’s New: A recent study focused on children whose M-CHAT screenings were negative, but who later received ASD diagnoses. The researchers examined data from more than 68,000 children collected as part of the Norwegian Mother and Child Cohort Study to look for children who passed the screening at 18 months but later received a diagnosis of ASD.
The researchers found:
- 228 of the children who screened negative ultimately received ASD diagnoses, constituting “false negatives.”
- Both boys and girls in the false negative group were rated as less social, less communicative, and having diminished gross motor skills compared to their counterparts in the true negative group. These effects were larger among girls, who constituted 16 percent of false negatives.
- Boys and girls in the false negative group were also shown to have diminished fine motor skills and to be less sociable than their counterparts in the true negative group.
- While boys in the false negative group were more shy than boys in the true negative group, the opposite was true of girls.
- No difference was found between the false and true negative groups in terms of emotionality and activity.
Why it’s important: This is the first study to establish a profile of “false negatives” for the M-CHAT screening. Future research
Help me understand :
| Source(s) : |
| Tweet |
Face-recording App May Screen for Autism
By Chelsea Toledo, M.A. on June 25, 2018

Background: Recent years have seen a huge surge in the number of apps created for Autism Spectrum Disorder (ASD), with the current number in the Apple app store topping 1,000. Many of these apps are aimed at instilling academic and functional skills in individuals with ASD. Others help users find support and services or provide news and raise awareness about ASD.
What’s New: A new study explored the use of an app for screening children with ASD. The researchers developed an iPhone app to detect differences in emotions and attentiveness – two areas affected in ASD. The app recorded the reactions of children as they watched movies on an iPhone, and then coded their behaviors. In all, 1,756 families with children between the ages of 1 and 6 years old participated over the course of a year, resulting in 4,441 videos of children in their natural settings. In addition, 5,618 demographic surveys were received from caregivers.
The researchers found:
- 32 percent of the participants were high risk for ASD, as defined by either having a caregiver report an ASD diagnosis having a high score on the M-CHAT ASD screening.
- Video clips - which included bubbles, bunnies, mirrors, and toys and songs - were each watched by more than half of the participants.
- Girls who were high risk for ASD demonstrated significantly less attention to the videos on bubbles, bunnies, and mirrors than girls who were low risk for ASD. This association was not the same for boys.
- Children with high M-CHAT scores were less likely to have positive emotional reactions to the bubbles movie than their peers with lower scores.
Why it’s important: This study suggests that app-based method could one day be leveraged to help screen for ASD in children. Because the screening would take place in children’s home environments, the results could be more meaningful than in-office interactions.
Image Credit: Kaethe Richter Henning, University of New Mexico, downloaded from the NIH Image Gallery under a Creative Commons license
Help me understand :
| Source(s) : |
| Tweet |
Reactions to Robot Could Reveal Internal Patterns in Autism
By Chelsea Toledo, M.A. on June 7, 2018

Background: Biologically speaking, a genotype is an organism’s underlying genetic identity, made up of inherited factors. A phenotype refers to observable characteristics such as social behavior. An intermediate term endophenotype is used to define stable, measurable traits, observed in multiple individuals, with a clear link to underlying genetic makeup.
What’s New: A new study assessed whether artificial intelligence could help reveal endophenotypes of individuals with Autism Spectrum Disorder (ASD). The researchers leveraged a female android robot, known as ACTROID-F, to interact with a total of 46 individuals representing four groups – adolescents (ages 13-17) with ASD, typically developing adolescents, young children (ages 1-5) with ASD, and typically developing young children. The robot was programed to smile, nod, move her eyebrows, and demonstrate other evidence of humaneness while interacting with the participants as they completed various tasks. The researchers administered a questionnaire to the adolescent participants and to the parents of the young children, measuring the degree to which the participants felt that the android displayed humaneness (i.e., whether their impression of her was natural, positive, competent, kind, conscious, human-like, responsible, nice, friendly, intelligent, and biological). They found that scores varied significantly between the participants with ASD and their typically developing peers.
Why it’s important: This study suggests that artificial intelligence could reveal an endophenotype for people with ASD. Further research could provide more information about the underlying genetic causes for these patterned differences.
Help me understand :
| Source(s) : |
| Tweet |
Future Autism Diagnosis Linked to Early Medical Conditions
By Shana R. Spindler, Ph.D. on May 30, 2017

Background: Early intervention for autism leads to fewer autism symptoms later in childhood. Unfortunately, autism diagnosis usually doesn’t occur until after three years of age. To improve time to therapy, researchers are looking for clues to diagnose autism as early as possible.
What’s new: In a large medical record study of 3,911 children with autism, researchers found that 38 medical conditions were associated with a future autism diagnosis. Medical conditions that showed the strongest link to autism included:
- Language delays
- Learning and cognitive disorders
- Global delays (significant delay in two or more areas of development)
- Motor delays
- Attention Deficit/Hyperactivity Disorder (ADHD)
- Anxiety disorders
- Cerebral palsy
- Epilepsy and recurrent seizures
- Disorders of the central nervous system
A combination of language delay with global delay most strongly correlated with an autism diagnosis. In total, the researchers identified 14 combinations of medical conditions that were associated with a future autism diagnosis.
Why it’s important: This study offers evidence that early life medical conditions could help doctors identify children who need close follow-up for autism assessment. Many of these medical conditions appear a year or more before autism symptoms become apparent.
Help me understand :
| Source(s) : |
| Tweet |
Simple iPad Game May Help Identify Children with ASD
By Shana R. Spindler, PhD on August 30, 2016

Background: More than 70 years ago, Dr. Leo Kanner described the abnormal social behaviors and movements of children with autism. Since then, many researchers have focused on the social features of the disorder. But motor control is important for many aspects of social and cognitive function. Now, several lines of evidence have shown that motor problems are present from a very young age in children who have Autism Spectrum Disorder (ASD).
What’s new: For the first time, researchers showed that hand movements on an iPad differ in children with ASD. In the study, researchers collected movement data as 37 children with ASD and 45 typically developing children played two simple iPad games. The researchers wrote a computer program that could learn from the movement data to predict if a child had ASD. Using the program, the researchers predicted ASD with up to 93% accuracy. In particular, they found that children with autism had greater contact force—how hard you press something with your finger—and larger movements with faster speed.
Why it’s important: To date, researchers can’t predict autism with high accuracy without expensive behavior monitoring. While the current study is only proof-of-concept, the results suggest that focusing on motor differences may allow researchers to identify early signs of ASD. A simple iPad game is an attractive option for screening or supplementing ASD diagnosis.
Help me understand :
| Source(s) : |
| Tweet |
ASD Risk Increases in Very Premature Babies
By Chelsea E. Toledo, M.A. on July 12, 2016

Background: Recent data from the U.S. Centers for Disease Control and Prevention shows that about 1 in 67 of 8-year-olds – or 1.5 percent – have an autism spectrum disorder (ASD) diagnosis. Boys are about four times more likely than girls to receive a diagnosis. The disorder, usually diagnosed during childhood, is characterized by social, behavioral and communicative differences.
What’s New: In a new study published May 25, 2016, researchers found that the prevalence of ASD was much higher – at about 7 percent – in children who were born before 27 weeks gestation. The risk of meeting ASD diagnostic criteria was higher the earlier a child was born.
The researchers performed an ASD screening on 889 10-year-olds who had been born at 23-27 weeks gestation, as well as follow-up diagnostic interviews on eligible children who met the screening criteria. They found that 61 children in the eligible sample met the diagnostic criteria for ASD, resulting in a prevalence of 7.1% in the entire group. The risk of meeting ASD diagnostic criteria increased the more prematurely children were born, with a prevalence of 15% in children born at 23-24 weeks gestation. About twice as many boys than girls met the diagnostic criteria for ASD.
Why it’s important: The overall prevalence of ASD was much higher in this sample of children born prematurely than in general population – with a much smaller ratio of boys to girls receiving diagnoses. This study suggests that children born prematurely should receive enhanced screening for ASD. Future studies could determine the underlying factors putting premature children at a greater risk.
Help me understand :
| Source(s) : |
| Tweet |
Newborns at Risk for Autism Differ in Social Preferences
By Shana R. Spindler, Ph.D. on June 9, 2016

Background: Newborn babies pay close attention to relevant social cues, such as a mother’s face. Some researchers hypothesize that the social preferences typically seen in infancy are impaired in autism, leading to an underdevelopment of “social brain” networks.
What’s new: On May 20, 2016, Scientific Reports published a study that examined social preferences in newborns at high risk for autism. The researchers showed social and non-social images to 13 newborns with high risk of autism and 16 newborns with low risk of autism—all between 6 and 10 days old. Researchers scored each newborn on how much he or she looked at the social versus non-social images. According to the report, the newborns at high risk for autism looked significantly more at the non-social images than the low-risk infants did.
Why it’s important: This is the first study to show that babies at high risk for autism show diminished social attention as early as 6 days after birth. Future research could include a larger number of infants and follow up to see if the high-risk infants receive an Autism Spectrum Disorder diagnosis.
Help me understand :
| Source(s) : |
| Tweet |
Eye-Tracking Tool May Detect ASD in Adults
By Chelsea E. Toledo, M.A. on May 3, 2016

Background: Autism spectrum disorder (ASD) is characterized by differences in communication, social interaction and behavior. A key indicator for ASD in infants and toddlers is abnormal gaze, as people with ASD tend to focus on different objects or movements than their typically developing peers. For example, someone with ASD would be less likely to make eye contact with another person as he or she spoke.
What’s New: On March 23, 2016, the journal Molecular Autism explored the use of an eye-tracking system called Gazefinder, which was developed to detect ASD in toddlers. The researchers showed scenes from movies to a study group of 26 males with ASD between the ages of 15 and 41 and a comparable group of individuals with typical development. Measuring the time participants’ eyes were fixated on a particular object or motion, researchers found that the ASD group spent significantly less time focused on socially significant objects or movements. For example, when looking at the face of a person sitting silently, the ASD group was more likely to focus on the mouth, as opposed to the typically developing group, who focused on the eyes.
Why it’s important: Atypical gaze is already a screening indicator for ASD in infants and toddlers. However, this study provided a concrete measure to distinguish much older people with ASD from their typically developing peers. Future research could explore the efficacy of this technique in females and in older children.
Help me understand :
| Source(s) : |
| Tweet |
Diagnosis Differences in Adopted Population with ASD
By Shana R. Spindler, Ph.D. on March 15, 2016

Background: Previous studies have linked adoption to general neurodevelopmental risks, but little is known about adoption as a risk factor for Autism Spectrum Disorder (ASD) specifically.
What’s new: In the February 2016 issue of the journal Pediatrics, researchers published a study exploring the differences in ASD diagnosis between adopted and non-adopted individuals. Using data in the Autism Speaks Autism Treatment Network, the researchers analyzed the cognitive ability, diagnosis, behavioral problems, and sleep habits for 163 adopted children and 5624 non-adopted children on the spectrum. They found that adopted children had increased:
- Attention problems
- Attention Deficit/Hyperactivity Disorder diagnosis
- Use of psychotropic medications
- Anxiety
- Depression
- Sleep problems
- Use of sleep medications
Why it’s important: This is the largest study of adopted individuals with autism to date. These results highlight the need for additional research in this unique subgroup, with a focus on factors associated with adoption—such as birth parent history, age at time of adoption, and history of institutionalization.
Help me understand :
| Source(s) : |
| Tweet |
Lost Diagnoses May Affect Autism Prevalence Estimates
By Chelsea E. Toledo, M.A. on December 30, 2015

Background: The U.S. Centers for Disease Control and Prevention estimates that 1 in 68 American children has autism spectrum disorder (ASD), a number based on nation-wide surveys and the review of medical and/or educational records. When public health professionals update survey design, the estimated autism prevalence often shifts to a different number. The actual prevalence is less defined than it may seem.
What’s New: On October 20, 2015, the journal Autism published a study exploring the possibility that estimates of ASD’s prevalence may be influenced by “lost diagnoses” – meaning that experts count children who previously had a diagnosis for autism that was later reconsidered. The researchers compared national survey data and retrospective parental interviews from 1420 children between the ages of 6 and 17 with ASD against those from 187 of their peers who had lost their diagnoses.
They found that about one in eight children ever diagnosed with ASD eventually lost the diagnosis, and that three-fourths of those diagnoses changed based on new information from doctors. According to the parental interviews, other reasons included:
- Initial diagnosis of ASD enabled the child to receive needed services, but the child never had ASD
- Treatment helped the condition go away
- Misdiagnosed after not testing properly
- Disagreement with the doctor’s diagnosis
Children with lost diagnoses were less likely to have parents concerned early on about their communication, behavior and social abilities, and were also less likely to have received their initial diagnosis from an ASD specialist.
Why it’s important: This study highlights the imprecise nature of autism estimates by pointing out several reasons for a lost ASD diagnosis. Future research could determine whether diagnoses made by non-specialists are overinflating the estimates of ASD prevalence.
Help me understand :
| Source(s) : |
| Tweet |
Four Key Trends Found for ASD Traits and Recurrence
By Shana R. Spindler, Ph.D. on November 5, 2015

Background: Several studies suggest that in families containing one or more individuals with Autism Spectrum Disorder (ASD), non-diagnosed members have increased presence of ASD-related traits. However, little is known about the prevalence or nature of these traits among the siblings in families where multiple members have ASD.
What’s new: On October 27, 2015, the journal Molecular Autism published a study exploring autism symptom pattern and recurrence in families with children on the spectrum. The researchers compared data for over 5500 siblings from the Autism Interactive Network. By examining single versus multiple incidence of ASD in a family, as well as the affected gender, the researchers discovered four key trends:
- Non-diagnosed children who have more than one sibling with autism possess an increased and specific pattern of autistic traits—namely resistance to change and restricted interests.
- Children with ASD from multiple incidence families are less symptomatic than those from single incidence families.
- A history of language delay with atypical speech is a risk factor for both social and restrictive/repetitive behavior symptoms in children not diagnosed with ASD from single or multiple incidence families.
- Males who are born into a multiple incidence family including at least one female with ASD are at a greater risk for possessing autistic traits. Likewise, families containing any number of females with ASD have greater recurrence risk for future children.
Why it’s important: This study may useful for the genetic counseling of families with ASD who are considering having another child, or for parents who are worried about their children’s risk of having a child with ASD. The study supports the idea that females require a greater risk factor burden before entering into an ASD diagnosis, making it more likely that males in the same family will have more severe autistic traits. It’s important to note, though, that currently there is no way to predict if anyone will or will not have a child with ASD or ASD-related traits.
Help me understand :
| Source(s) : |
| Tweet |
Researchers Create Rapid ASD Screening for Toddlers
By Chelsea E. Toledo, M.A. on August 25, 2015

Background: Autism Spectrum Disorder (ASD) is typically diagnosed via behavioral observation of a child. The American Academy of Pediatrics currently recommends that children undergo a “level one” screening at their 18- and 24-month well visits. If that screening, which involves questions about a child’s communicative and social behaviors, raises a concern about ASD, the child is usually referred to a specialist who can conduct more formal assessments.
What’s New: On August 15, 2015, the Journal of Pediatrics published a study detailing a new screening tool for toddlers. The researchers administered the ten-minute, play-based test, called Rapid Interactive Screening Test for Autism in Toddlers (RITA-T) to a total of 61 toddlers, including 42 with developmental concerns established by a level one screening. RITA-T was 88 percent accurate in predicting the 23 ASD diagnoses ultimately made through formal diagnostic tests.
Why it’s important: RITA-T has the potential to become a useful “level two” screening tool for clinicians, helping to weed out the false positives generated by level one screenings and allowing for earlier diagnosis and intervention.
Help me understand :
| Source(s) : |
| Tweet |
Sensorimotor Differences in ASD Appear in Infancy
By Chelsea E. Toledo, M.A. on August 4, 2015

Background: In the United States, one in 68 children is estimated to have Autism Spectrum Disorder (ASD). Children who have an older sibling with the disorder face a much higher risk, which studies have estimated to be about one in 10. Researchers can study these infants and toddlers at high risk of ASD to learn about the early onset characteristics of autism.
What’s New: On July 16, 2015, The Journal of Neurodevelopmental Disorders published a study exploring differences in behavioral, cognitive, and adaptive development among infants at high and low risk of developing ASD. The researchers performed established screenings to assess the behavior of 308 children—210 of whom were high-risk and 98 of whom were low risk for ASD—at 6, 12 and 24 months of age. They classified 49 of the high-risk children as having ASD at 24 months, with the children who most closely matched the profile demonstrating sensorimotor deficits at 6 months of age. In contrast, the less severely affected children displayed their first differences in the form of socio-communication skills by two years of age.
Why it’s important: Previous studies on infants have revealed differences first appearing in social and communicative abilities. This finding—that children most severely affected by ASD have early sensorimotor difficulties—could reveal some of the physiological basis for the disorder, leading to earlier diagnosis and intervention.
Help me understand :
| Source(s) : |
| Tweet |
Diagnosis Swap May Increase ASD Prevalence
By Shana R. Spindler, Ph.D. on July 28, 2015

Background: Autism Spectrum Disorder (ASD) is characterized by impaired social and communication skills and the presence of restrictive or repetitive behaviors. The United States Centers for Disease Control (CDC) estimates the current prevalence of ASD at 1 in 68 children. This is a sharp increase from the CDC estimate of 1 in 150 children with ASD in 2002.
What’s new: On July 22, 2015, the American Journal of Medical Genetics published a study comparing the prevalence of ASD with other comorbid conditions, such as intellectual disability (ID), among 6.2 million children enrolled in special education programs in the United States. The researchers report that a decrease in ID diagnosis accounts for about 64 percent of the increase in autism prevalence between 2002 and 2010. Age of the child appears to influence the re-categorization of diagnosis, with older children seeing a greater shift toward autism diagnosis than younger children.
Why it’s important: These data suggest that healthcare professionals are using the diagnosis of ASD in place of comorbid classifications more often, and this accounts, in part, for the increase in ASD rates over the last decade.
Help me understand :
| Source(s) : |
| Tweet |
Study Paves Way for Blood Test for Autism
By Chelsea E. Toledo, M.A. on June 2, 2015

Background: To date, trained clinicians diagnose Autism Spectrum Disorder (ASD) by structured behavioral observation of a child. The typical age of ASD diagnosis is between the ages of four and five in US children. However, research has shown that interventions performed earlier in life lead to better outcomes in children with the disorder.
What’s New: On April 1, 2015, JAMA Psychiatry published a study testing the effectiveness of genetic biomarkers in the blood to predict whether very young children would receive an ASD diagnosis. The researchers first looked for factors differentiating the blood of 147 male children between the ages of one and four—56 with typical development and 91 who were diagnosed with ASD by their third birthday. They identified a genetic signature related to the body’s immune response that was 83 percent accurate at predicting whether participants had ASD. The researchers were able to replicate their findings in a separate group of 73 children, which included 44 boys with ASD.
Why it’s important: This study provides proof of the principle that immune-related gene expression differs in people with ASD. Future work could lead to a blood test to screen for the disorder in children as young as one year old, allowing for earlier intervention.
Help me understand :
| Source(s) : |
| Tweet |
Researchers Probe Blood Biomarkers for ASD
By Chelsea E. Toledo, M.A. on February 9, 2015

Background: At present, the only way to diagnose autism spectrum disorder (ASD) is through a series of behavioral screenings administered by trained professionals. While no laboratory test for ASD is currently available, recent studies have suggested that certain features detected in the blood could prove reliable as biomarkers for the disorder.
What’s new: The January 2015 issue of Neuroscience included a study evaluating two components in blood, serotonin and interleukin-6, as biomarkers for detecting ASD. While serotonin helps to regulate mood, interleukin-6 plays a role in the body’s inflammatory response to invading pathogens. The researchers performed blood tests on a total of 66 individuals—35 with ASD and 31 with typical development—whose average age was 12. They found that levels of serotonin and interleukin-6 were significantly elevated in the individuals with ASD, and were highest in those with the most severe forms of the disorder.
Why it’s important: The study found that, when taken together, serotonin and interleukin-6 were very reliable biomarkers for ASD—as blood tests looking for both molecules were accurate nearly 90 percent of the time. This work could lead to a clinical blood test for ASD risk, and could point the way to treatments targeting serotonin and interleukin-6.
Help me understand :
| Source(s) : |
| Tweet |
Brief Observations Unreliable for ASD Diagnosis
By Chelsea E. Toledo, M.A. on January 22, 2015

Background: Although studies have identified differences in children with autism spectrum disorder (ASD) appearing as early as infancy, the behavior of very young children with ASD could match that of typically developing counterparts at times. With age, atypical behaviors appear with increasing frequency in children with ASD. This pattern is potentially problematic for families seeking early diagnosis, as the behavioral observations considered in clinicians’evaluations of children are usually quite brief.
What’s new: The February 2015 issue of Pediatrics included a study exploring the efficacy of brief behavioral observations for identifying children with ASD. The researchers conducted evaluations for a total of 44 children between the ages of 15 and 33 months, administering multiple questionnaires and observations to assign them to one of three groups: ASD, language delay, and typical development. Two psychologists specializing in early childhood development then watched 10- to 30- minute videos of the children to make their own evaluations. The researchers found that the experts were unable to catch 39 percent of the ASD cases from the brief observations alone, as the children with ASD demonstrated typical behavior 89 percent of the time.
Why it’s important: This is the first study to measure the extent to which young children with ASD can exhibit typical behavior. It suggests that any atypical behaviors appearing in observations merit follow-up and additional screening.
Help me understand :
| Source(s) : |
| Tweet |
Autism Increase Attributed to Reporting Practices
By Chelsea E. Toledo, M.A. on January 13, 2015

Background: The United States Centers for Disease Control and Prevention estimates that 1 in 68 American children will receive a diagnosis of autism spectrum disorder, or ASD. The rate has increased significantly since autism first appeared in the Diagnostic and Statistical Manual of Mental Disorders in 1980.
What’s new: The January issue of JAMA Pediatrics featured a study examining autism prevalence in Denmark, where rates of ASD have also increased. Because of the country’s nationalized health system, the researchers were able to examine the records of all 677,915 Danish children born between 1980 and 1991, following up until 2011. They determined that two-thirds of the increase in ASD rates could be attributed to changes in the diagnostic criteria in 1994 and the inclusion of diagnoses from outpatient facilities in 1995.
Why it’s important: This is the first large-scale study to quantify the effect changes in reporting practices have on ASD rates. Future research could determine the cause of the increase not explained by changes in reporting practices, as well as the generalizability of these findings to other countries, such as the United States.
Help me understand :
| Source(s) : |
| Tweet |
Researchers Search for Autism Blood Test
By Chelsea E. Toledo, M.A. on November 15, 2014

Background: Studies have shown that children with autism spectrum disorder (ASD) experience better outcomes the earlier they receive a diagnosis. Using currently available assessments—which include evaluations of language, behavior, and intellectual abilities—clinicians diagnose children with ASD at the average age of four.
What’s new: On November 7, 2014, the open-access journal PLoS One featured a study exploring techniques to find markers for ASD in the blood of affected individuals. The researchers compared the blood plasma of 39 children with ASD to that of 22 typically developing peers and found 179 features differentiating their blood. Using five different laboratory tests, the scientists tested for those same features in the blood of another set of children—13 with ASD and 8 with typical development—and were able to accurately classify them more than 80 percent of the time.
Why it’s important: This study moves the field closer to having a blood test for ASD, which would allow for earlier diagnosis and intervention. Future studies could refine which combination of biomarkers and which laboratory tests result in the most accurate diagnosis.
Help me understand :
| Source(s) : |
| Tweet |
ASD Diagnosis Increased with Additive Risk Factors
By Chelsea E. Toledo, M.A. on September 23, 2014

Background: Some researchers hypothesize that autism stems from a single causal event that initiates a cascade of cognitive and developmental delays. In contrast, others hypothesize that autism is the cumulative result of several co-existent risk factors. Studies have shown that disparities in social attention in children as young as 10 months old can predict whether those children later receive an ASD diagnosis, especially if they have an older sibling with ASD. Separate research has evaluated non-social attention—for example, how quickly a child can shift focus from one stimulus to another—and found differences in children as young as 6 months old, depending on their level of risk for developing ASD. By utilizing social and non-social attention tasks, researchers hope to learn about autism’s initial causes.
What’s new: The July 2014 issue of Developmental Science included a study assessing both social and non-social attention in children at 13 months of age. Using data from previous studies evaluating the two factors separately, the researchers combined data collected from a total of 145 children who had either undergone a task to follow the gaze of a person shown on a screen or the task to shift focus from one stimulus shown on a screen to another. They found that disparities in social and non-social attention had cumulative effects in predicting an ASD diagnosis—that is, infants who followed the gaze of the person on the screen for short periods of time and who also took long periods of time to shift from one task to another had a higher chance of developing ASD than those who scored better on each task.
Why it’s important: This is the first study to formally test the relationship between multiple factors (i.e. social and non-social attention) as they relate to the development of ASD. This research paves the way for future studies to more conclusively determine whether ASD develops due to cumulative risk, as this study suggests, or from a single causal factor.
Help me understand :
| Source(s) : |
| Tweet |
Possible Autism Biomarker in Tiny Regulators
By Shana R. Spindler, PhD on September 10, 2014

Background: Several studies have shown that early intervention helps children with Autism Spectrum Disorder (ASD) improve critical social and language skills. Unfortunately, doctors still lack a non-behavioral clinical test to find out if a child has or will develop ASD. Diagnosis is therefore delayed until the child reveals social or language deficits, usually by two to four years of age. Researchers are now searching for autism biomarkers, an objective measurement that can predict the likelihood that a child has autism, even before behavioral symptoms used for diagnosis appear.
What’s new: A group of Japanese researchers report in Molecular Autism that a new class of small gene regulators, called microRNAs (miRNAs), may help predict ASD. The team of scientists found that individuals with autism had higher levels of eight specific miRNAs in serum samples compared to control individuals. In contrast, five miRNAs showed lower levels in those with autism. MicroRNAs are like little zip ties that bind gene products to control the cell from making certain proteins. The researchers identified several proteins involved in neuron biology among the protein targets affected by the miRNAs in this study.
Why it’s important: To date, the medical community lacks a biomarker of any type for autism. This is the first study to show that specific miRNAs are found at different levels in the serum of those with autism versus controls. Serum collection is a relatively safe and noninvasive procedure. These results suggest that the measurement of serum miRNAs may serve as a biomarker for autism, but additional studies are needed to confirm this finding.
Help me understand :
| Source(s) : |
| Tweet |
Disorder-Specific Screening Catches More ASD Cases
By Chelsea E. Toledo, M.A. on March 20, 2014

Background: The American Academy of Pediatrics recommends that physicians screen all children for autism spectrum disorder (ASD) beginning at 18 months of age (http://www.cdc.gov/ncbddd/autism/hcp-recommendations.html). However, while most pediatricians routinely administer tests for a broad spectrum of developmental disorders, very few report that they screen specifically for ASD.
What’s New: The February 2014 issue of the journal Autism presents a study (originally published online December 21, 2012), comparing the ability of two types of screening tools to detect ASD in young children. The researchers evaluated 52 children between 18 and 24 months of age, using the Parents Evaluation of Developmental Status (PEDS) and Modified Checklist for Autism in Toddlers (MCHAT), as well as the updated M-CHAT with follow-up interview (M-CHAT+FUI). All participants then underwent diagnostic evaluation, resulting in 30 ASD diagnoses. While the broad PEDS screening caught 17 of those cases, the M-CHAT and M-CHAT+FUI detected 28 and 27, respectively.
Why it’s important: From the results, the researchers concluded that a combination of broad and disorder-specific screenings provide optimum detection of ASD cases, allowing for early intervention for those children ultimately diagnosed with ASD. However, with the release of the Diagnostic and Statistical Manual of Mental Disorders-Fifth Edition in May 2013, the diagnostic criteria for ASD shifted. Future studies will need to address how the new requirements for ASD affect the success of screening tools.
Help me understand :
| Source(s) : |
| Tweet |
DSM-5 Criteria May Reduce ASD Prevalence, Slightly
By Shana R. Spindler, Ph.D. on January 30, 2014

Background: On May 18, 2013, the American Psychiatric Association released the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), providing guidelines for mental disorder identification. The previous version, DSM-IV-TR, used a three-domain approach to diagnose autism, including criteria for social interaction, communication deficits, and repetitive or restrictive behaviors. In contrast, the DSM-5 measures two domains—social aspects and repetitive behavior. Moreover, DSM-5 focuses on the range of symptoms and severity under a single Autism Spectrum Disorder (ASD) compared to specific subtypes, such as Autistic Disorder and Asperger syndrome, outlined in DSM-IV. These controversial changes have led some to question if the new version will catch all autism cases, which ultimately affects autism prevalence rates as well as access to therapy.
What’s new: In a population-based study, a collection of United States researchers found that DSM-5 criteria likely captures about 81 percent of existing autism cases. The researchers analyzed patient records from the Autism and Developmental Disabilities Monitoring (ADDM) network, a large multi-site surveillance system in the United States.
Of the 644,883 records assessed, a total of 6,577 records showed an ASD diagnosis using DSM-IV-TR criteria. When the researchers applied DSM-5 criteria to those same records, only 5339 patients still had ASD. Children with regressive history or intellectual disability and children who had originally been diagnosed by a community professional were more likely to meet all DSM-5 requirements. Surprisingly, 304 of 1020 children received an ASD diagnosis with DSM-5 criteria after narrowly missing an autism diagnosis according to DSM-IV-TR guidelines.
Why it’s important: Unlike previous clinic-based studies, the current study used a population-based system to examine how DSM-5 will affect autism prevalence, hopefully providing a more accurate assessment. Given that as much as 19 percent of autism diagnoses may change with the DSM-5 criteria, future studies examining changes in autism prevalence will need to take this into account.
Help me understand :
| Source(s) : |
| Tweet |
Updated Screening Tool Helps Provide Early ASD Diagnosis
By Chelsea E. Toledo, M.A. on January 15, 2014

Background: Early intervention has been shown to have positive outcomes for children with autism spectrum disorder (ASD). However, the disorder is typically diagnosed in children over the age of four, with an average age of diagnosis ranging from 38 to 120 months for all ASDs. During the last decade, researchers developed a screening assessment that could be administered at toddlers’ regular medical check-ups, with the aim of facilitating earlier diagnosis.
What’s new: On December 23, 2013, the journal Pediatrics published a study evaluating an updated version of that screening tool—called the Modified Checklist for Autism in Toddlers, Revised with Follow-up (M-CHAT-R/F). The researchers administered the 20-question checklist—which assessed children’s physical, social, and communicative habits—to parents of 16,071 children at their 18- and 24-month well-child care visits. Based on the responses, children were classified as low-, medium-, or high risk—with a follow-up questionnaire to refine the classification of those allocated to the medium-risk category. One percent of the children were ultimately deemed high-risk and were referred for further evaluation. Of those, 95 percent had confirmed developmental delays, and 47.5 percent received ASD diagnoses.
Why it’s important: From the results, the researchers concluded that the updated version of the M-CHAT is better at detecting ASD than its previous iteration. At the same time, the newer version of the screening tool classifies a smaller proportion of children as high- or medium-risk—reducing the number of families who would need to pursue follow-up testing.
Help me understand :
| Source(s) : |
| Tweet |
Blood Test Distinguishes Those with Autism
By Shana R. Spindler, Ph.D. on January 6, 2014

Background: Today, doctors diagnose Autism Spectrum Disorder (ASD) using behavioral evaluation, limiting how early in development a doctor can detect signs of autism. For this reason, researchers are looking for autism biomarkers, measurable features that are predictive of the disorder. One line of research investigates how much genes are turned on or off in the body. Called a “gene expression profile,” this particular measurement could distinguish children with ASD.
What’s new: Using DNA chip technology, researchers at Boston Children’s Hospital and Harvard Medical Center analyzed gene expression profiles in the blood cells of 20 pairs of siblings, in which only one sibling had ASD, and 18 unrelated control individuals. According to their study, 189 genes differed in expression between the affected and unaffected siblings. Surprisingly, a small group of the unaffected siblings had gene expression profiles that more closely matched the unrelated individuals than their own sibling. The genes that differed in expression are known to play a role in cell maintenance, energy production, neural signaling, immune response, and calcium signaling pathways.
Why it’s important: This study supports the idea that gene expression profiles may help predict if a child will develop autism. This has implications for early diagnosis, or at the very least, the identification of children that may need closer monitoring of developmental progress. Additional studies with larger sample sizes are needed to verify the study’s findings.
Help me understand :
| Source(s) : |
| Tweet |
Eye Fixation is Lost, Not Absent, in ASD
By Shana R. Spindler, Ph.D. on November 15, 2013

News Brief: A new article in the high impact journal Nature has received a lot of coverage in the media recently, for good reason. United States researchers revealed that poor eye contact observed in children with Autism Spectrum Disorder (ASD) results from a gradual decline in eye fixation in two to six-month-old infants. Their findings suggest a potential window for early intervention in ASD before this social behavior is lost. It remains unclear, however, if addressing eye fixation deficits will improve other ASD-related behaviors.
Help me understand :
| Source(s) : |
| Tweet |
Team Approach Still Gold Standard for ASD Diagnosis
By Shana R. Spindler, Ph.D. on October 10, 2013

Background: A multidisciplinary approach that incorporates clinical evaluations and behavioral observations has been the gold standard for Autism Spectrum Disorder (ASD) diagnosis. Given the cost and time associated with multiple evaluations, researchers are investigating if a lean model of diagnosis that utilizes fewer assessments can diagnose ASD equally well.
What’s new: Researchers at the Gillberg Neuropsychiatry Centre in Gothenburg, Sweden, designed a study to find which autism assessments best diagnose ASD or if a multidisciplinary approach is still needed. The researchers compared independent assessments for 34 children age 24 to 46 months using psychiatric evaluation, Griffiths’ Developmental Scales, language assessment, the Diagnostic Interview for Social and Communication disorders (DISCO), the Autism Diagnostic Observation Schedule (ADOS), and preschool/home observation. After completion of the independent assessments, the clinicians held a diagnostic case conference for each child to deliver a final diagnosis.
Of the six assessments examined in the study, the most informative was the preschool/home observation, while the psychiatric evaluation matched poorest with the final diagnosis. No single assessment type was perfect, and this especially held true for female children. Based on the poor agreement between individual assessments, the researchers suggest that a comprehensive clinical evaluation should remain the gold standard for ASD diagnosis.
Why it’s important: Families and insurance providers rely on studies like these to determine which diagnostic assessments are necessary for proper care. Given the findings in this study, a comprehensive evaluation that utilizes multiple assessment types likely offers the best care to date.
Help me understand :
| Source(s) : |
| Tweet |
Parent-Rated Measure Comparable to Established Test
By Chelsea E. Toledo, M.A. on August 28, 2013

Background: Most assessments for autism spectrum disorder (ASD) assess social skills, communicative abilities, and repetitive behaviors. The Autism Treatment Evaluation Checklist (ATEC), administered by parents, tests for ASD’s physical manifestations as well, but has not been extensively evaluated against standard ASD diagnostic tools.
What’s new: On July 3, 2013, a study comparing ATEC to a more established assessment measure was published online in the Journal of Mental Health Research in Intellectual Disabilities. The researchers administered the Child Autism Rating Scale (CARS)—a well-established test for ASD severity—to 56 children aged 2 to 16. Participants’ parents then completed the ATEC survey, which elicited information about the children’s communicative levels, sociability, sensory awareness, and physical behavior. They found a significant association between participants’ scores on the ATEC and CARS measures. However, larger studies are needed to validate this tool.
Why it’s important: This study provides support for the utility of parent-rated ATEC measure to assess ASD. Because the test includes physical criteria, it could provide a more complete picture of children affected by ASD. You can complete the ATEC online at http://www.surveygizmo.com/s3/1318614/Autism-Treatment-Evaluation-Checklist.
Help me understand :
| Source(s) : |
| Tweet |
New Tool Provides Potential Screening and Treatment
By Chelsea E. Toledo, M.A. on August 9, 2013

Background: Most assessments for autism spectrum disorder (ASD) are based on a person’s behavior. However, children with ASD are known to display unpredictable patterns of physical movement—a possible target for more personalized autism screening and therapy.
What’s New: On July 24, 2013, the journal Frontiers in Integrative Neuroscience featured a set of studies exploring physical movements as a target for assessing and treating ASD. In the first study, the researchers assessed how 34 individuals with ASD and 44 typically developing control subjects followed cues to point at objects on a screen over a series of trials. They found disruptions in the progress of individuals with ASD as trials ensued. In the second study, the researchers tested the ability of 25 individuals with ASD and 8 control subjects to hold an arm within a desired area. They found that, when provided a reward—the chance to watch an enjoyable video, autistic subject’s movements became more predictable, suggesting that self-discovery tasks can improve anticipatory behavior.
Why it’s important: Fifteen years ago, Teitelbaum et al. showed movement disturbances as integral component of autism that could be clearly detected as early as 4 – 6 month old infants. These two new studies could bring the value of movement analysis in evaluating ASD to the forefront.
Help me understand :
| Source(s) : |
| Tweet |
Overlapping Disorders Can Inform Autism Symptoms
By Chelsea E. Toledo, M.A. on June 6, 2013

Background: In clinical settings, health professionals have noted overlaps between autism spectrum disorder (ASD) and various other childhood syndromes, such as attention deficit hyperactivity disorder (ADHD). A leading child psychiatrist, Christopher Gillberg, proposed a model in 2010—called Early Symptomatic Syndromes Eliciting Neurodevelopmental Clinical Examinations (ESSENCE)—in which a range of disorders affecting childhood development would be considered and addressed simultaneously.
What’s New: On March 25, 2013, the Scientific World Journal published a retrospective study of 413 adults with various psychiatric disorders. Their parents reported the impairments they faced in early development—including difficulties in communication, motor skills, social interaction, and other areas. As children, individuals with either ASD or ADHD, or both disorders, reportedly faced greater difficulties in nearly all areas than those with other disorders.
Why it’s important: This study suggests that developmental disorders like ADHD and ASD are linked to a range of problems with behavior and development. Using the ESSENCE model, the researchers identified symptoms that professionals do not use to diagnose ASD or ADHD, such as gross and fine motor skills, body and visual perception, memory, and time concepts, to name a few, but that can nevertheless shed light on the complexity those disorders present.
Help me understand :
| Source(s) : |
| Tweet |
Autism Linked to Atypical Visual Attention in Infancy
By Chelsea E. Toledo, M.A. on April 18, 2013

Background: Along with its hallmark social and communicative impairments, autism spectrum disorder (ASD) is commonly associated with a narrow focus of attention and interest. Studies of autistic adults have demonstrated that they experience increased activation in brain areas known for processing local versus global information—a pattern linked to superior performance on detail-oriented tasks.
What’s New: On January 29, 2013, the journal Biological Psychology featured a study of visual attention in infants, and its relation to ASD diagnoses later in life. The researchers videotaped 104 infants between six and 15 months of age as they watched animations either in the center of a screen or in its periphery. They found that the infants who were later diagnosed with ASD were more likely than their typically developing peers to continue focusing on the center of the screen after an animation moved to the periphery, and that they displayed inconsistent speed and flexibility in visual orientation.
Why it’s important: This study suggests that infants who develop autism have atypical development of visual attention beginning in the first year of life. However, infants who were later diagnosed with other developmental syndromes showed similar patterns in visual attention, underscoring possible overlaps in childhood disorders.
Help me understand :
| Source(s) : |
| Tweet |
Child’s Facial Features May Predict Autism Diagnosis
By Shana R. Spindler, PhD on February 22, 2013
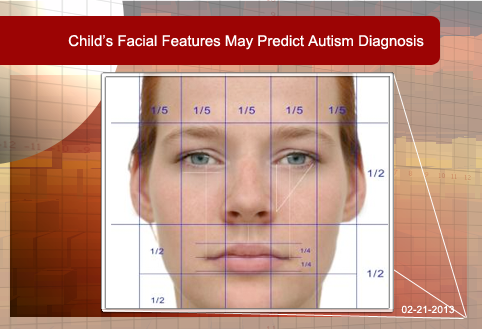
Background: Genes, small sections of DNA that code for proteins, control how the body develops and functions. Autism Spectrum Disorder (ASD) is known to have a strong genetic component. Some of the genes that contribute to autism may also help shape body and facial features. Researchers hypothesize that certain physical characteristics may predict an autism diagnosis.
What’s New: Researchers at University Medical Center in Utrecht, The Netherlands, and at the University of California, Los Angeles, discovered that facial asymmetry, abnormal hair whorls, and a prominent forehead are highly predictive of ASD in a Caucasian population. None of the abnormalities, however, linked to a specific ASD subgroup, such as Autistic disorder or Asperger syndrome. The collaborators published their findings in the January 2013 issue of the Journal of Autism and Developmental Disorders.
Why it’s important: Many doctors believe that early intervention can positively affect behavioral outcomes in children with autism, and evidence supports this claim. To date, the only way to diagnose autism is through careful observation of a child’s behavior. The current study suggests that the measurement of specific physical features may become a tool used by doctors to help predict an ASD diagnosis before behavioral problems arise.
Help me understand :
| Source(s) : |
| Tweet |
Blood Test Could Aid Autism Diagnosis
By Chelsea E. Toledo, M.A. on January 9, 2013

Background: Over the past few decades, the rate of diagnosis for Autism Spectrum Disorder (ASD) has increased to about 1 in 88 children. While studies have shown that early diagnosis is linked to better cognitive outcomes in children with ASD, most children are not diagnosed until after they reach the age of 4, according to the Centers for Disease Control. This is due in part to limited diagnostic tools, such as traditional interviews and observation-based evaluations.
What’s New: On December 5, 2012, the online journal PLoS ONE published the largest study to date of blood biomarkers as a diagnostic target for ASD. The researchers identified a set of 55 genes that were expressed differently in the blood of 66 autistic males when compared to 33 of their typically developing counterparts. They then ran a blood test seeking those same genes out in 104 children with ASD and 82 without the disorder. The test achieved an accurate diagnosis 70 percent of the time overall, predicting 73 percent of cases in male children and 51 percent of cases in female children.
Why it’s important: While a blood test may not replace traditional diagnostic evaluations for ASD, the authors speculate that their method could reduce the time spent determining whether a child has the disorder, allowing for earlier intervention. This study’s small sample size and inadequate accuracy rate, however, warrant the need for additional research.
Help me understand :
| Source(s) : |
| Tweet |
Parents of Children with ASD Want Genetic Testing
By Stacy W. Kish on December 14, 2012
Background: The diagnosis of Autism Spectrum Disorder (ASD) by behavioral observations often comes years after the parents suspect a problem with their child’s development. However, children diagnosed at a younger age can begin receiving interventions that show improvement in language skills, adaptive behavior, and IQ scores. Parents with one child diagnosed with ASD report increased rates of anxiety for their younger children.
What’s new: Genetic testing is a major area of focus in ASD. In this study, researchers surveyed parents with at least one autistic child to gather parents’ input on their interest in a genetic test. Overwhelmingly, 80 percent of parents with one autistic child would consider genetic testing if it becomes available to help establish the risk of the disorder in younger children. Parents also seek clear and honest answers from their doctors.
Why it’s important: Parents are interested in a genetic test that could indicate risk of ASD, even if the test cannot confirm a diagnosis. Diagnosing children at a younger age improves intervention treatments and parental acceptance of the diagnosis.
Help me understand :
| Source(s) : |
| Tweet |
Health Care Providers Create Autism Clinical Database
By Stacy W. Kish on December 6, 2012

Background: The Centers for Disease Control and Prevention estimates that 1 in 88 children have been diagnosed with some component of autism spectrum disorder (ASD). ASD describes a group of symptoms associated with abnormal brain development. Previously, researchers established the Interactive Autism Network (IAN), an internet-based registry. The network, however, required parents to self-register their child and fill out forms.
What’s new: Kaiser Permanente and Harvard Pilgrim are pooling data retrieved from electronic medical records to create one of the largest autism database to date. Using these resources, the health care providers identified 20,000 people with ASD. Unlike similar networks, this database contains standardized information that will aid researchers as they study the disorder.
Why it’s important: The clinical and scientific community can use this data to understand the prevalence of ASD and current methods used to treat symptoms. In addition, researchers could comb the database to recruit individuals for clinical trials. Finally, organizations hope to develop autism awareness campaigns to help educate underserved communities about the condition. The database will not become available to researchers until privacy issues associated with medical records are resolved.
Help me understand :
| Source(s) : |
| Tweet |
Cord Blood Testosterone Level Fails to Predict ASD
By Mark N. Ziats on November 14, 2012

Background:
More males than females are diagnosed with autism, at a rate of at least 4:1. This significant gender difference, along with previous animal and human studies of sex differences in brain development, has led researches to speculate that children with Autism Spectrum Disorder (ASD) may be exposed to more testosterone—the chief male sex hormone—than unaffected children.
What’s new:
In a study published in the Journal of Neurodevelopmental Disorders on 30 October 2012, researchers measured testosterone in the umbilical cord blood of 707 newborns and then followed the cohort for 20 years to determine if the testosterone level at birth correlated with a future diagnosis of ASD or presence of autistic traits. The researchers found that testosterone levels were not associated with an ASD diagnosis nor related to the development of autistic-like traits in those subjects without a diagnosis of autism. However, only five of the 707 newborns developed autism. A follow-up study with greater numbers is important to validate these findings.
Why it’s important:
This research suggests that the level of testosterone at birth does not correlate with the development of autism. Additional studies are needed to determine if testosterone levels during the early stages of pregnancy play a role in ASD risk.
Help me understand :
| Source(s) : |
| Tweet |
Home Videos Reveal Early Autism-Related Behaviors
By Chelsea E. Toledo, M.A. on November 9, 2012

Background: By the time they reach school age, children with Autism Spectrum Disorder (ASD) are known to differ from developmentally delayed (DD) children in their patterned reactions to various stimuli. However, less is known about how those patterns of hyporesposiveness—or a lack of response to stimuli—and hyperresponsiveness—or an extreme response to stimuli—manifest when those children are younger than school age.
What’s New: In a report published in the American Journal of Occupational Therapy, researchers detail a qualitative study of home videos featuring 12 children—six with ASD and six with DD. From the videos, which were taken when the children were between 0 and 2 years old, the researchers discerned behaviors associated with hyporesponsiveness and hyperresponsiveness, as well as sensory repetitions such as mouthing objects. They found that children in the ASD group displayed patterns not present in the DD group: The children either remained hyporesponsive from infancy to school age, or they shifted from hyporesponsive behaviors to sensory repetition as they aged.
Why it’s important: Studies have shown that early diagnosis and intervention for ASD yields positive outcomes for the affected children. Further research on sensory patterns in infants and toddlers could implicate hyporesponsiveness as a behavioral precursor for ASD, leading to an earlier diagnosis.
Help me understand :
| Source(s) : |
| Tweet |
Computational Method May Aid Autism Diagnosis
By Chelsea E. Toledo, M.A. on October 23, 2012

Background: Recent technological advances have the potential to improve how Autism Spectrum Disorders (ASD) are classified and diagnosed. Brain cells use energy when they communicate with each other, which results in increased blood flow to their local area to replenish their energy. Scientists use a technique called functional magnetic resonance imaging (fMRI) to measure these changes in blood flow, allowing them to infer which areas of the brain are active.. Computational approaches are then used to help find patterns of activated brain regions, allowing ASD patient brain activity patterns to be compared to those of neurotypical patients.
What’s new: In a study published in the October 2012 edition of the online journal PLoS ONE, researchers detail an emerging computational approach for analyzing fMRI data from 58 people—half of whom had an ASD diagnosis. They monitored the activity of 106 brain regions and found their method could distinguish ASD patients in >80% of the cases. Additionally, the researchers found that an ASD diagnosis could better be predicted at a fine scale rather than at a coarse scale (involving long-range connections between different brain regions) that researchers typically look at.
Why it’s important: Many scientists believe that ASD is associated with the way regions of the brain interact with one another, but few have been able to demonstrate concretely how those problems manifest. Better ways of analyzing brain images could lead to a better understanding of how ASD works—and how it can be remedied.
Help me understand :
| Source(s) : |
| Tweet |
New Autism Guidelines Catch Most Cases
By Chelsea E. Toledo, M.A. on October 17, 2012

Background: The Diagnostic and Statistical Manual of Mental Disorders (DSM), published by the American Psychiatric Association, provides criteria for identifying mental and behavioral syndromes. The current edition, DSM-IV, contains a three-domain model for diagnosing Autism Spectrum Disorder (ASD), based on criteria for social interaction, communication and behaviors. The newly proposed criteria for ASD, to be published in DSM-V, have two domains for diagnosis—social interaction and behavior, with communicative criteria now considered part of social interaction.
What’s New: Studies evaluating the new ASD criteria have been limited in discerning their sensitivity—how accurately they diagnose people with ASD—as well as their specificity—how well they distinguish between people with ASD and those with other disorders. In a report published in the American Journal of Psychiatry, researchers describe a new study of over 5,000 children evaluated by way of observations and interviews with their parents. The study reports that the DSM-V criteria for ASD were as sensitive and more specific than those in DSM-IV—resulting in correct diagnoses 91 percent of the time.
Why it’s important: Previous studies have suggested that the proposed criteria for ASD could exclude many people with Asperger syndrome or pervasive developmental disorder-not otherwise specified (PDD-NOS). Without diagnoses, people with ASD could lose access to care. However, the new guidelines catch most cases of both syndromes.
Help me understand :
| Source(s) : |
| Tweet |
Specific Genetic Variations May Help Predict ASD
By Shana R. Spindler, Ph.D. and Mark Ziats on October 12, 2012

Background: The diagnosis of Autism Spectrum Disorder (ASD) is currently based on clinical interviews. Doctors lack laboratory tests or other biomarkers to help support a diagnosis. Autism has a strong genetic component, but knowing which genetic variations contribute to or protect against autism is a major challenge for diagnosis.
What’s new: Scientists have developed a diagnostic test by mapping genetic variations into cellular pathways that might be affected in autism. A specific combination of 237 common genetic variations, called single nucleotide polymorphisms (SNPs), can predict an ASD diagnosis with at least 71 to 85 percent accuracy, according to a new study published 11 September in Molecular Psychiatry. The predictive accuracy, however, is only strong in those genetically similar to Central Europeans. The same SNPs predicted ASD with only 57 percent accuracy in a genetically dissimilar Chinese population. According to the authors, at least some of the genes harboring autism-linked SNPs are expressed in various brain regions implicated in ASD, and those genes are also important for cellular processes required for proper neuron functioning.
Why it’s important: An SNP profile may eventually become an important biomarker in the diagnosis of ASD. SNP testing during early infancy could allow detection of ASD before symptoms manifest, allowing for earlier therapeutic intervention, which may increase the success rate of therapy.
Help me understand :
| Source(s) : |
| Tweet |
Researchers Study Eye Tracking in Natural Environment
By Stacy W. Kish on October 9, 2012

Background: One characteristic of Autism Spectrum Disorder (ASD) is the avoidance of making or maintaining eye contact. Instead, autistic children tend to focus on they eyebrows, mouth, or other facial features. Scientists hypothesize that avoiding eye contact narrows the development of the social brain network.
What’s new: Unlike previous studies set in a clinical setting, this study examined the gaze of autistic and typically developing children in a natural environment. Each child wore a device to monitor their gaze as s/he responded to and engaged in normal forms of play. During these interactions, the researchers measured the direction of gaze and the child’s field of vision. The autistic children in the study avoided the face of the experimenter more than children in the control group did. The autistic children also used their lateral field of view and looked downward more than the control group.
Why it’s important: Researchers study the gaze of autistic children to understand how the disorder affects child development. Studies in a natural setting are rare, and this work provides a unique perspective in this area of research. Future work could build on these findings by studying how head motion and focus on non-social stimuli could lead to development of novel diagnostic tools
Help me understand :
| Source(s) : |
| Tweet |
New Autism Study Recruiting Newborns
By Chelsea Toledo, M.A. on October 2, 2012
Background: Autism Spectrum Disorder (ASD) is typically diagnosed in early childhood. The rates of diagnosis have increased in recent years—from 2006 to 2008 its prevalence increased by 23 percent, with 1 in 88 children being diagnosed in the United States. Studies have shown that ASD is more commonly diagnosed in boys, and that 20 percent of children with ASD will have a sibling with the disorder.
What’s New: The National Institutes of Health have awarded a 5 year, .2 million grant to The Center for Autism Research at the Children's Hospital of Philadelphia (CHOP) for a study on children starting at 3 months old. The researchers are currently recruiting expecting parents and parents of newborns with or without a family history of ASD. Using magnetic resonance imaging (MRI), they aim to pinpoint early signs of ASD by observing changes in the children's brains from infancy to 5 years of age.
Why it’s important: Earlier research at CHOP demonstrated that autistic children's brains develop differently than those of children without the disorder. These internal differences emerge before the disorder becomes externally apparent. Children who receive timely interventions for autism have better life outcomes, so understanding the early changes in the brain could lead to quicker diagnosis and more effective therapy.
Help me understand :
| Source(s) : |
| Tweet |
Autism Associated with Family Mental Health History
By Chelsea E. Toledo, M.A. on September 13, 2012

Background:
Until the 1980s, Autism Spectrum Disorder (ASD) was commonly diagnosed as childhood schizophrenia. Although ASD and schizophrenia are now regarded as distinct, common causal factors—such as genetic variations—can contribute to either condition, as well as to bipolar disorder.
What’s New:
In the 2 July 2012 online edition of the journal Archives of General Psychiatry, researchers report that ASD appears more frequently in people whose parents or siblings have been diagnosed with schizophrenia or bipolar disorder. The researchers studied over 30,000 medical records from Sweden and Israel and found that ASD was three times more likely to occur in people whose parents had a schizophrenia diagnosis. For people whose siblings had schizophrenia, ASD appeared 2.5 times more often in the Swedish group and 12 times more often in the group from Israel. In the entire sample, ASD was about twice as likely to occur when either a sibling or a parent was diagnosed with bipolar disorder.
Why it’s important:
The understanding of ASD’s cause remains incomplete. By studying factors that make ASD more common in some families than in others, researchers gain greater knowledge of the disorder’s etiology.
Help me understand :
| Source(s) : |
| Tweet |
Effectiveness of Sensory Integration Therapy Unknown
By Catherine Croft Swanwick, Ph.D. on May 28, 2012

Background: Sensory-based therapies are increasingly used for neurodevelopmental disorders such as autism, but the American Academy of Pediatrics now cautions parents about the lack of research regarding their effectiveness. Many autistic children are overly sensitive to sensory input (i.e., sound, light, touch). Sensory–based therapies aim to help them cope with these sensitivities in daily life.
What’s New: The lack of data about sensory integration therapy spurred the council of pediatricians to make three main recommendations, summarized here:
- At this time, pediatricians should not use sensory processing disorder as a diagnosis. Instead, when sensory symptoms are present, other neurodevelopmental disorders should be considered.
- Pediatricians should recognize and communicate with families about the limited data on the use of sensory-based therapies for childhood developmental and behavioral problems.
- Pediatricians can teach families to evaluate the effectiveness of sensory-based therapies, such as with trial periods and monitoring techniques.
Why It’s Important: Although sensory-based therapy may be acceptable as one component of a comprehensive treatment plan, parents and pediatricians should closely monitor its effects.
Help me understand :
| Source(s) : |
| Tweet |
Diagnoses Vary According to Doctor
By Shana R. Spindler, Ph.D. on November 21, 2011
Pop News Brief: Recently highlighted in Fox news, a study published November 7, 2011, in the online Archives of General Psychiatry reported that the proportion of diagnoses for different autism spectrum disorders varied across 12 University-based sites, even though the sites had similar distributions of patient scores based on standardized measures. The authors of the study suggest that a diagnosis should consist of “dimensional descriptions” of core features rather than the common sub-grouping categories used today.
Help me understand :
| Source(s) : |
| Tweet |
Low Birthweight Linked to Autism
By Shana R. Spindler, Ph.D. on November 10, 2011

Background: According to a new study, children born at a low birthweight may be at an increased risk for developing autism. Researchers at the University of Pennsylvania School of Nursing and School of Medicine followed over 1100 infants who weighed less than 4.4lbs at birth to the age of 21 by periodic assessment.
What's new: The group reported in the Oct 17 online edition of Pediatrics that an estimated 5% of children born under 4.4lbs will go on to develop Autism Spectrum Disorder (ASD). The researchers followed low-birthweight infants to age 21, likely capturing both severe and mild forms of ASD.
Why it's important: According to the Centers for Disease Control, 1% of 8-year-old children have ASD, indicating that a low birthweight may increase a child’s risk of developing the disorder by five-fold.
Help me understand :
| Source(s) : |
| Tweet |

